Vasectomy and Laser Precision in Vas Occlusion
Vasectomy has long been recognized as one of the most reliable and permanent methods of male contraception. Traditionally, this minimally invasive procedure involves blocking or cutting the vas deferens—the small tubes that carry sperm from the testicles to the urethra. However, in recent years, medical technology has redefined how vas occlusion is performed. Among the most promising innovations is laser precision in vasectomy, which enhances control, reduces trauma, and improves patient recovery outcomes.
The integration of laser systems into urological surgery represents a transformative shift, combining accuracy with minimal invasiveness. In this article, we’ll explore how laser precision is changing vasectomy techniques, the science behind laser occlusion, its benefits, safety profile, and what patients can expect from this cutting-edge approach.
Understanding the Basics of Vasectomy
A vasectomy involves the surgical interruption of the vas deferens to prevent sperm from entering the semen. The procedure is typically performed under local anesthesia and takes less than 30 minutes. Conventional vasectomy techniques include:
- Ligation and excision: Cutting and tying off the vas deferens.
- Cauterization: Sealing the vas deferens using heat.
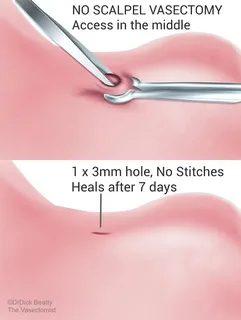
- No-Scalpel Vasectomy: Using a small puncture instead of an incision to access the vas deferens.
While these methods are highly effective, they depend heavily on surgical skill and mechanical precision. This is where laser-assisted vasectomy steps in, offering a level of accuracy and control that manual methods cannot match.
The Role of Lasers in Modern Vasectomy
Lasers have become integral in modern medicine, especially in ophthalmology, dermatology, and oncology. Their inclusion in vasectomy procedures represents a similar evolution—where precision and tissue preservation are equally prioritized.
In a laser-assisted vasectomy, surgeons use a focused laser beam to occlude or seal the vas deferens. The laser’s energy precisely targets the inner lumen of the vas, causing controlled coagulation that closes the duct without excessive heat spread or tissue damage.
Different types of lasers can be used, including:
- Diode lasers: Common for soft-tissue applications, providing accurate energy delivery.
- CO₂ lasers: Offer high precision and minimal collateral damage.
- Nd:YAG lasers: Penetrate deeply, ideal for creating durable occlusion.
These systems are integrated with imaging guidance, giving surgeons real-time feedback during vas occlusion, further improving success rates.
Laser Precision: How It Works in Vas Occlusion
Laser occlusion in vasectomy is a process of thermal fusion—where concentrated energy seals the vas lumen. The technique involves three core steps:
- Target Identification:
The surgeon isolates the vas deferens using micro-instruments or through a no-scalpel approach. - Laser Application:
A laser probe delivers short pulses of energy that heat and collapse the inner wall of the vas. The precision of the beam ensures that only the intended tissue is affected, reducing the chance of collateral damage. - Sealing and Verification:
The sealed section of the vas is checked for integrity using imaging tools like high-resolution micro-ultrasound or infrared visualization, ensuring complete closure.
Unlike traditional cauterization, laser precision avoids excessive charring or scarring, maintaining cleaner tissue planes. This reduces postoperative pain and speeds up recovery.
Advantages of Laser Precision in Vasectomy
1. Enhanced Surgical Accuracy
The greatest benefit of laser-assisted vasectomy lies in its ability to deliver sub-millimeter accuracy. The focused laser beam allows surgeons to isolate and seal the vas deferens with remarkable precision, reducing human error.
2. Minimal Tissue Trauma
Because lasers cause localized heating, there is less damage to surrounding structures such as nerves and blood vessels. This leads to a lower risk of hematoma, infection, or prolonged pain.
3. Shorter Recovery Time
Laser-based procedures promote faster healing and less inflammation. Many patients can return to normal activities within days, compared to a week or more for conventional methods.
4. Reduced Risk of Sperm Granuloma
Sperm granulomas—small nodules caused by sperm leakage—can occur when the vas is not properly sealed. Laser occlusion creates a uniform seal, significantly lowering this risk.
5. Better Cosmetic Outcomes
The use of a fine laser incision or puncture results in minimal scarring, improving aesthetic outcomes and patient satisfaction.
6. Improved Sterility Verification
Modern laser systems can be paired with optical coherence tomography (OCT) or infrared sensors to verify occlusion in real-time, ensuring near-zero failure rates.
Laser Vasectomy vs. Traditional Methods
| Feature | Traditional Vasectomy | Laser-Assisted Vasectomy |
| Incision Type | Small scalpel or puncture | Laser micro-incision |
| Tissue Damage | Moderate | Minimal |
| Bleeding Risk | Low | Very low |
| Precision | Manual | Computer-guided or robotic |
| Recovery Time | 5–7 days | 2–3 days |
| Pain Level | Mild to moderate | Minimal |
| Failure Rate | 1 in 2,000 | Potentially lower with guided imaging |
| Scarring | Small scar | Nearly invisible |
This comparison underscores how laser precision in vasectomy improves nearly every measurable surgical and patient-centered outcome.
Integration with Imaging and AI Systems
The new wave of smart surgical systems combines laser technology with AI-based imaging and robotic assistance. These platforms allow for:
- AI-driven anatomical mapping: Algorithms identify vas deferens with accuracy even in challenging anatomies.
- Laser energy modulation: The system automatically adjusts intensity based on tissue feedback to prevent overheating.
- Real-time analytics: Data from temperature sensors and imaging systems guide the surgeon in optimizing closure.
These integrations make laser vasectomy a step toward fully automated microsurgical sterilization, with the potential for unmatched precision and consistency.
Safety and Efficacy Profile
Laser technology in vasectomy has undergone early clinical evaluation, and the results are promising. Studies suggest:
- Efficacy rates exceed 99.9% in complete vas occlusion.
- Postoperative discomfort is 40–50% lower than with conventional cauterization.
- Return-to-work time averages 2.5 days, compared to 5–7 days traditionally.
Moreover, lasers eliminate the need for electrocautery, minimizing thermal spread and tissue necrosis. As more urology centers adopt these systems, long-term data will help refine best practices and standardize protocols.
Patient Experience and Recovery
Patients undergoing laser-assisted vasectomy report smoother recoveries. Typical post-surgery expectations include:
- Mild discomfort for 24–48 hours.
- Minimal swelling, usually managed with over-the-counter pain relief.
- Quick resumption of work and physical activity, often within three days.
Follow-up semen analysis remains essential to confirm sterility. The laser does not alter sperm production or hormonal function, ensuring that sexual function and testosterone levels remain unaffected.
Future Directions: Toward Smart, Scarless Vasectomy
The integration of laser precision marks the beginning of a larger transformation in reproductive surgery. Research is now exploring:
- Fully robotic vasectomy platforms that combine laser occlusion with automated imaging.
- Smart fiber lasers capable of self-adjusting to tissue resistance.
- Nano-laser-assisted sealing that could further minimize invasiveness.
- AI-driven predictive analytics to identify ideal occlusion energy thresholds for each patient.
These innovations point toward a future where vasectomy becomes a same-day, pain-free, and scarless procedure, performed with microscopic accuracy and instant confirmation of success.
Conclusion
The evolution of vasectomy from manual cutting and cauterization to laser precision in vas occlusion is a remarkable advancement in urological surgery. This technology brings together accuracy, safety, and patient comfort, reducing complications and speeding up recovery.
By integrating laser systems with imaging and AI, surgeons can now perform vasectomies with unparalleled precision—offering men a reliable, minimally invasive, and technologically enhanced form of permanent contraception.
As more clinics adopt these innovations, laser-assisted vasectomy is poised to become the new gold standard, ensuring consistent results and redefining male sterilization with modern medical science.
Frequently Asked Questions (FAQs)
1. How is laser-assisted vasectomy different from a traditional vasectomy?
In a traditional vasectomy, the vas deferens is manually cut and sealed using sutures or cautery. A laser-assisted vasectomy uses a focused laser beam to seal the vas with pinpoint accuracy, reducing tissue damage, pain, and recovery time.
2. Is laser vasectomy safer than conventional methods?
Yes. Laser vasectomy minimizes bleeding, infection, and postoperative pain due to its non-contact nature and precise thermal control. The targeted energy application ensures only the vas deferens is affected, protecting surrounding tissues.
3. How soon can I return to normal activities after a laser vasectomy?
Most patients can resume normal daily activities within two to three days after laser vasectomy. However, it’s recommended to avoid heavy exercise and sexual activity for about a week to allow proper healing and ensure effective occlusion.