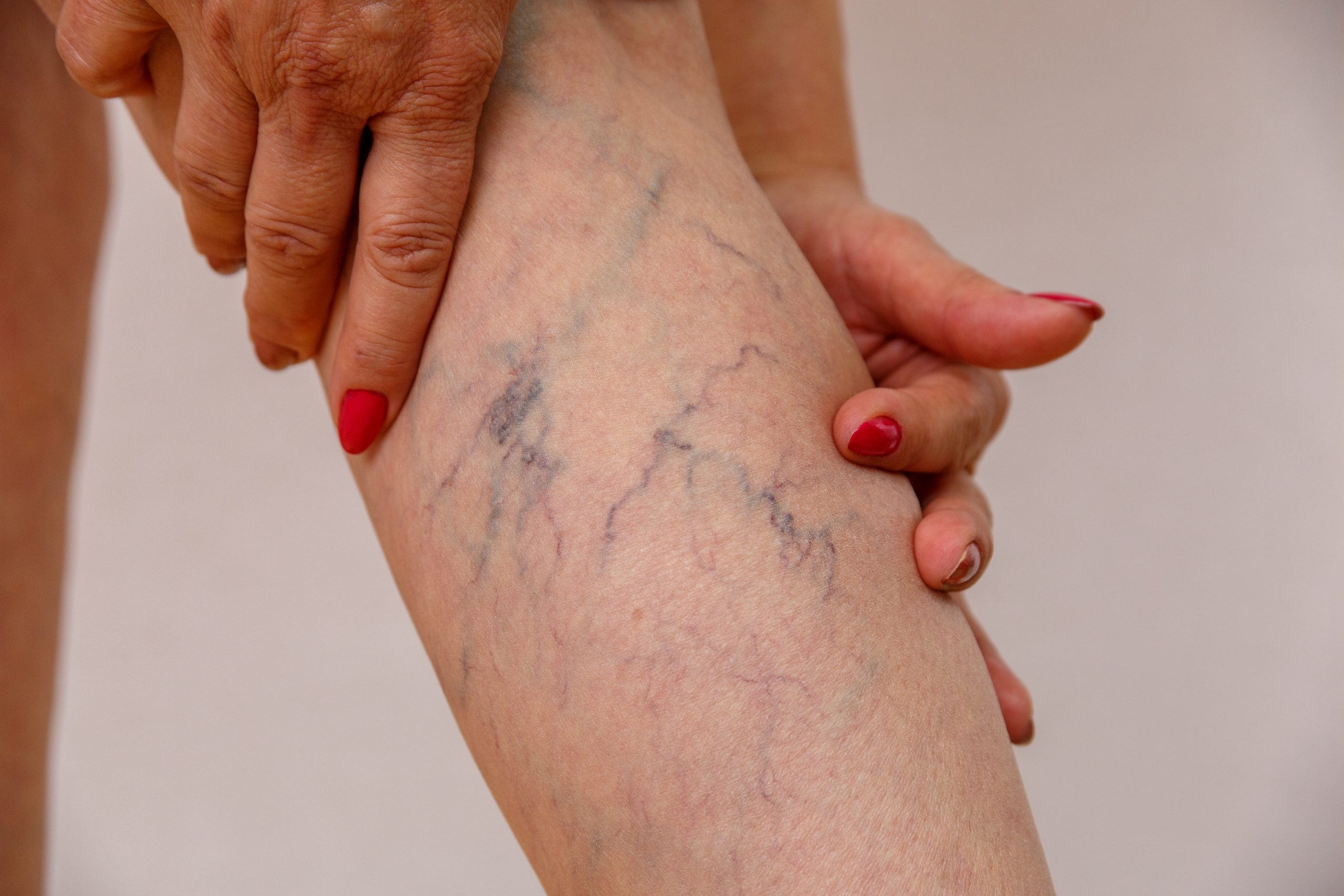
Does Insurance Consider Varicose Vein Treatment Medically Necessary or Cosmetic?
Varicose veins are not just a cosmetic concern—they can significantly impact your health and daily life. If you’ve noticed bulging veins in your legs, aching, or swelling, you might be wondering: are varicose veins covered by insurance? Many patients are unsure whether insurance providers classify vein treatment as medically necessary or cosmetic. Understanding this distinction can help you make informed decisions about treatment and potential out-of-pocket costs.
What Are Varicose Veins and Why Do They Matter?
Varicose veins are enlarged, twisted veins that often appear on the legs and feet. They occur when the valves in the veins weaken or fail, causing blood to pool instead of flowing efficiently to the heart. While some people may have no symptoms, others experience pain, swelling, heaviness, fatigue, or even skin ulcers in severe cases.
Even if varicose veins seem purely cosmetic, they can lead to serious health complications. Untreated varicose veins can cause chronic venous insufficiency, blood clots, or skin ulcers. For this reason, vein treatment is often considered more than just a cosmetic procedure in the medical community.
How Insurance Companies Decide if Treatment Is Medically Necessary
Insurance providers typically categorize medical procedures as either medically necessary or cosmetic. This classification directly impacts whether your policy will cover the costs.
- Medically Necessary Treatment: A treatment is considered medically necessary if it addresses a health condition that affects your daily life or prevents further complications. For varicose veins, this includes symptoms such as leg pain, swelling, skin changes, or the risk of blood clots.
- Cosmetic Treatment: Procedures are labeled cosmetic if they primarily improve appearance without addressing a health risk or functional problem. Vein treatments aimed solely at enhancing the look of your legs often fall into this category.
Insurance providers rely on documentation from your physician or a vein treatment clinic to determine the classification. This documentation usually includes a detailed report of symptoms, diagnostic tests such as ultrasound results, and the recommended treatment plan.
Are Varicose Veins Covered by Insurance?
The answer to are varicose veins covered by insurance? is nuanced. Coverage depends on the severity of your condition, your insurance policy, and whether the procedure is deemed medically necessary.
- Symptomatic Varicose Veins: If your veins cause pain, swelling, skin ulcers, or other complications, insurance is more likely to cover treatment. Procedures like endovenous laser therapy, sclerotherapy for problematic veins, or vein stripping may be reimbursed.
- Asymptomatic or Cosmetic Varicose Veins: If your veins are primarily a cosmetic concern, insurance coverage is usually denied. Treatments aimed purely at improving appearance are considered elective.
At Vein Treatment New Jersey, specialists carefully evaluate each patient to determine whether treatment meets medical necessity criteria. By providing thorough documentation and diagnostic evidence, patients improve their chances of insurance approval.
Factors That Influence Insurance Coverage
Several key factors affect whether insurance providers cover varicose vein treatment:
- Medical Documentation: Clear evidence of symptoms, failed conservative treatments (compression stockings, lifestyle changes), and complications can strengthen your claim.
- Diagnostic Imaging: Ultrasound or duplex vein scans are often required to confirm the presence of reflux or other venous issues.
- Insurance Policy: Each insurance plan has specific criteria for coverage. Some may require prior authorization or evidence that conservative treatments were unsuccessful.
- Type of Treatment: Minimally invasive procedures like radiofrequency ablation or endovenous laser therapy may have different coverage rules than surgical vein stripping.
Patients who meet these criteria typically have a higher chance of insurance approval, while those seeking treatment primarily for cosmetic purposes may need to pay out-of-pocket.
How to Maximize Your Chances of Insurance Approval
If you’re considering vein treatment and want insurance coverage, taking the right steps is essential.
- Consult a Specialist: Visiting a reputable vein treatment clinic ensures accurate diagnosis and proper documentation. Specialists can distinguish between medical necessity and cosmetic treatments.
- Document Your Symptoms: Keep a record of leg pain, swelling, ulcers, or bleeding. Photos of visible veins and detailed symptom descriptions help support your claim.
- Try Conservative Treatments First: Insurance providers often require patients to attempt non-invasive solutions such as compression stockings, exercise, or elevation before approving invasive procedures.
- Request Pre-Authorization: Many insurers require pre-approval for vein treatments. Submitting all medical records and diagnostic results upfront can expedite the process.
Following these steps increases the likelihood that insurance will cover your varicose vein treatment.
Types of Varicose Vein Treatments Insurance Might Cover
When treatment is deemed medically necessary, insurance may cover several options:
- Endovenous Laser Therapy (EVLT): A minimally invasive laser procedure to close damaged veins.
- Radiofrequency Ablation (RFA): Uses radiofrequency energy to heat and seal the vein.
- Sclerotherapy for Problematic Veins: Injection of a solution to collapse veins that cause pain or swelling.
- Vein Stripping and Ligation: Surgical removal of veins for severe cases.
Coverage may include associated costs like diagnostic imaging and follow-up visits, depending on your insurance plan.
When Treatment Is Likely Considered Cosmetic
Treatment is usually deemed cosmetic if the procedure addresses only the appearance of the veins without significant pain, swelling, or risk of complications. Procedures such as microphlebectomy for purely aesthetic purposes are rarely covered.
Insurance companies make this distinction to manage costs and prioritize treatments that address medical issues over elective cosmetic improvements.
Conclusion
Understanding whether varicose veins are covered by insurance is crucial before seeking treatment. Insurance coverage depends on medical necessity, documentation, and the specific policies of your insurer. By consulting a qualified vein treatment clinic like Vein Treatment New Jersey, documenting symptoms, and pursuing appropriate diagnostic evaluations, patients can increase their chances of coverage.
Ultimately, while some varicose vein treatments may be considered cosmetic, many are medically necessary and essential for improving health and preventing complications. Knowing your options and understanding insurance criteria allows you to make informed decisions for your vascular health.
If you are struggling with painful or problematic veins, consult Vein Treatment New Jersey today to determine your treatment options and whether your procedure could be covered by insurance.